The COVID-19 conversation to have now
(FOX 9)
(FOX 9) - Most Americans who get sick with COVID-19 will recover, but many, including the elderly and those with serious underlying medical conditions, may get very sick, very fast.
“It’s really the speed it’s happening that’s taking everyone by surprise,” said Dr. Keith Mortman, head of thoracic surgery at George Washington University Hospital in D.C.

The COVID-19 conversation to have now
Why experts say having hard conversations about your potential COVID-19 treatment plan is crucial, albeit difficult and uncomfortable.
Dr. Mortman developed a 3D virtual reality tour of the lungs of a 59-year-old man with COVID-19, based on a CAT scan. The image graphicly shows damaged tissue and fluid accumulating in the lungs, a condition known as Acute Respiratory Distress Syndrome (ARDS).
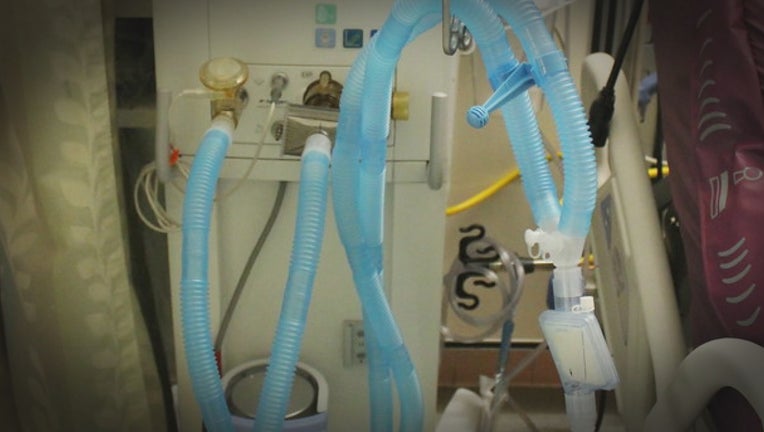
The patient was on a mechanic ventilator to help him breathe. He died, having never made it off the ventilator.
“Unfortunately, right now there is no treatment, there is no cure per se for COVID,” said Dr. Mortman.
“It’s a call to everyone to have those conversations now with loved ones, ‘Hey, if you were in this position, what would your wishes be?’”
‘Outcomes are sobering’
Ventilators simply buy time for the most critically ill patients, but often not enough time.
The patient is sedated with a tube inserted down the windpipe, pushing air into the lungs, filling up tiny sacs that oxygenate the blood.
Public health officials have feared there won’t be enough ventilators for all who need them to stay alive.
“If you need a ventilator, and don't get one, there is a very slim chance you are going to survive it,” said Governor Tim Walz in a State of the State address Wednesday.
Governor Walz repeated a statistic he has used often since the start of the pandemic. “If you do need a ventilator, and you get one, your chance of survival increases ten times,” said Walz.
But it is also true, based on studies in the United States, China, and Italy, that most COVID-19 patients who go on a ventilator will die.
“The outcomes are sobering,” said Dr. James Pacala, a geriatrician and head of Family Medicine at the University of Minnesota Medical School.
Dr. Pacala said compared with others who have ARDS, COVID-19 patients tend to stay on a ventilator longer, around two weeks to 20 days, which can permanently damage their lungs, heart, and lead to cognitive impairment.
The longer someone is on a ventilator, the less likely they will ever get off.
“Only about a third of the older adults who are on ventilators will get off of them,” said Dr. Pacala.
There is even discussion in the medical community about whether doctors, reacting to patients’ low blood oxygen levels, are using ventilators too often, when less invasive procedures would have better results.
The ‘Fair Innings’ Concept
The average age of those who have died from CoVid-19 in Minnesota is 87. Several computer models have predicted that about one percent of those infected, many of them older with underlying medical conditions, will need a ventilator.
On the front lines of the pandemic, in the nation’s hardest hit hospital ICU units, doctors are confronting a grim calculus of preserving resources like ventilators for those most likely to survive.
Some call it the ‘fair innings rule.’
“People younger, they deserve more of a chance,” explained Dr. Pacala of the thinking. “Whereas if you’re late in the baseball game you need to let someone play the game.”
COVID-19 has caused a huge paradigm shift in the American medical system.
“The default in everything in American health care is we will keep you alive as long as technologically possible,” said Professor Thaddeus Pope, director of the Health Law Institute at Mitchell Hamline School of Law.
He believes most patients and their families don’t understand the implications of being placed on a ventilator, and don’t anticipate that the patient will be sedated and unable to make medical decisions for themselves.
Professor Pope said there are two legal documents people should consider.
Advance Directive vs. Order for Treatment
Everyone should have an Advance Medical Health Care Directive, recommends Prof. Pope.
This is a document listing a person’s wishes and preferences during an assortment of medical scenarios, along with a designated decision maker if the person is incapacitated or sedated.
For those already seriously ill, Prof. Pope said it is important to have what’s known as a Provider (or Physician) Order for Life Sustaining Treatment (POLST).
Rather than a listing of preferences, a POLST is an actual legal order making it explicitly clear what heroic measures should be taken, or more likely not taken, to save your life.
It is a way for patients with already serious medical conditions, who are unlikely to survive, to say, “Don’t waste this scarce ventilator on me. Give it to someone who may have better prospects,” said Pope.
If things get desperate, and resources scare, doctors will likely be making these decisions anyway.
Several hospitals on the East Coast have considered blanket ‘Do Not Resuscitate’(DNR) orders for COVID-19 patients.
Asked if Minnesota hospitals might consider such an order, a spokesperson for the Minnesota Hospital Association said hospitals are waiting for guidance from the Minnesota Department of Health (MDH).
Resources for the Discussion
But if there is a conversation to be had in your family, about quality of life, and the ‘big picture,’ the experts say the time to talk is now, before a loved one is hospitalized and unable to communicate.
These are complicated and deeply personal issues for families to grapple with, and there are some resources that are good starting points for the discussion.
The Minnesota Medical Association has an updated COVID-19 guide for those seeking a Provider Order for Life Sustaining Treatment (POLST), including an FAQ, talking points for having a conversation, specific guidance for those entering an assisted living (AL) and skilled nursing facility (SNF), and POLST forms in several languages.
Other resources available include Honoring Choices Minnesota, an Advance Care Planning Initiative led by the foundation for the Twin Cities Medical Society. They have instructional materials as well as forms for health care directives and POLST orders in several languages.
The Minnesota Department of Health (MDH) has a question and answer section on health care directives.
There is also a group based in California, Prepare for Your Care, that has updated guidance and information specifically tailored to the COVID-19 pandemic, with instructional videos and medical directive forms in ten languages.

