Four out of five autoimmune disease patients are women. New study reveals why
Diabetes patient checks blood pressure. Type 1 diabetes is one of the most common autoimmune diseases. (Photo By BSIP/UIG Via Getty Images)
Up to 50 million Americans have an autoimmune disease – a condition in which your immune system attacks healthy cells – and as many as 80% of those people are women.
A new study led by researchers at Stanford Medicine has figured out why: it’s the X factor.
There are more than 80 types of autoimmune diseases, according to the National Library of Medicine. The most common are type 1 diabetes, multiple sclerosis, rheumatoid arthritis, lupus, Crohn’s disease, psoriasis and scleroderma.
According to Stanford researchers, the women-men ratio for lupus is 9 to 1; for Sjogren’s syndrome, it’s 19 to 1. The disparity, they say, stems from "the most fundamental feature differentiating biological female mammals from males."
They hope the new discovery can lead to a better way to predict autoimmune disorders before they develop.
RELATED: Cancer cases increasing in US, but overall deaths decreasing, new research shows
"As a practicing physician, I see a lot of lupus and scleroderma patients, because those autoimmune disorders manifest in skin," Howard Chang, MD, PhD, professor of dermatology and of genetics and a Howard Hughes Medical Institute investigator, said in a statement. "The great majority of these patients are women."
What are autoimmune diseases?
Multiple sclerosis is an autoimmune disease affecting central nervous system. (Photo by: BSIP/Education Images/Universal Images Group via Getty Images)
According to the National Library of Medicine, the immune system protects you from disease and infection by attacking germs that get into your body, like viruses and bacteria.
When you have an autoimmune disease, your immune system mistakes healthy cells in your organs and tissues for foreign invaders and attacks them.
RELATED: 'Disease X': Scientists creating contingency plan for infectious virus outbreak
Autoimmune diseases can affect almost any part of your body, and they’re the third leading cause of chronic illness in the United States, according to the National Stem Cell Foundation.
The prevalence of autoimmune diseases is increasing, though researchers don’t know why.
Why women are at greater risk of autoimmune disease
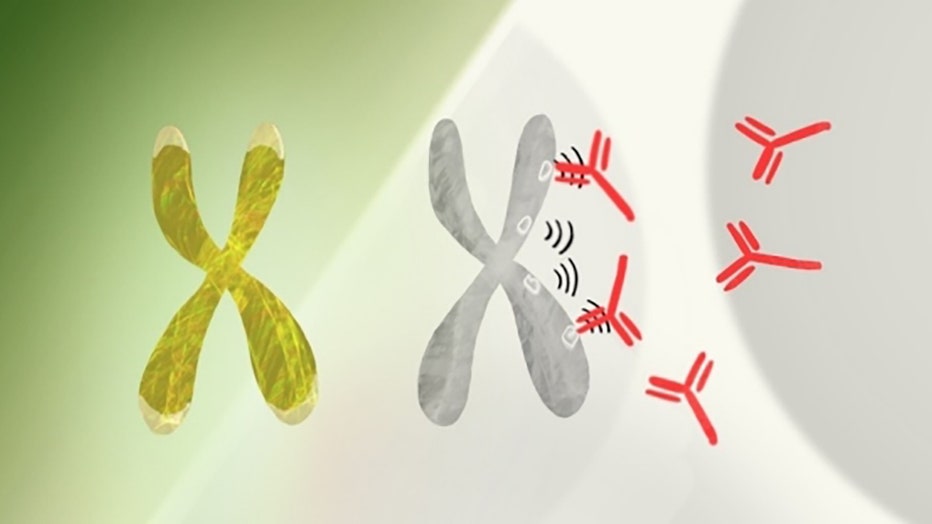
In every cell in a woman’s body, one X chromosome is disabled to ensure that the right levels of proteins are produced from that chromosome pair. But the way the second chromosome is shut down generates unfamiliar molecular structures that can trigge
Stanford researchers say it boils down to women having too much of a good thing: the X chromosome. Females have two X chromosomes while males have one X and one Y.
The new research, published in the journal Cell, shows that extra X is involved — but in an unexpected way.
Our DNA is carried inside each cell in 23 pairs of chromosomes, including that final pair that determines biological sex. The X chromosome is packed with hundreds of genes, far more than males’ much smaller Y chromosome. Every female cell must switch off one of its X chromosome copies, to avoid getting a toxic double dose of all those genes.
Performing that so-called X-chromosome inactivation is a special type of RNA called Xist, pronounced like "exist." This long stretch of RNA parks itself in spots along a cell's extra X chromosome, attracts proteins that bind to it in weird clumps, and silences the chromosome.
RELATED: Skin aging, wrinkles may be linked to bacteria on your face, study suggests
Chang was exploring how Xist does its job when his lab identified nearly 100 of those stuck-on proteins. Chang recognized many as related to skin-related autoimmune disorders — patients can have "autoantibodies" that mistakenly attack those normal proteins.
"That got us thinking: These are the known ones. What about the other proteins in Xist?" Chang said. Maybe this molecule, found only in women, "could somehow organize proteins in such a way as to activate the immune system."
If true, Xist by itself couldn’t cause autoimmune disease or all women would be affected. Scientists have long thought it takes a combination of genetic susceptibility and an environmental trigger, such as an infection or injury, for the immune system to run amok. For example, the Epstein-Barr virus is linked to multiple sclerosis.
Chang’s team decided to engineer male lab mice to artificially make Xist — without silencing their only X chromosome — and see what happened.
Researchers also specially bred mice susceptible to a lupus-like condition that can be triggered by a chemical irritant.
The mice that produced Xist formed its hallmark protein clumps and, when triggered, developed lupus-like autoimmunity at levels similar to females, the team concluded.
"We think that’s really important, for Xist RNA to leak out of the cell to where the immune system gets to see it. You still needed this environmental trigger to cause the whole thing to kick off," explained Chang, who is paid by the Howard Hughes Medical Institute, which also supports The Associated Press’ Health and Science Department.
Beyond mice, researchers also examined blood samples from 100 patients — and uncovered autoantibodies targeting Xist-associated proteins that scientists hadn't previously linked to autoimmune disorders. A potential reason, Chang suggests: standard tests for autoimmunity were made using male cells.
The Associated Press contributed to this report.

